|
Table of Content - Volume 21 Issue 2 - February 2022
Clinical profile of anaemia with special reference to neurological changes at tertiary hospital
Neelima S Deshpande1*, Babita M Yadav2, Sudhir Deshmukh3
1Professor & HOD, Department of Medicine, 3Dean, Vilasrao Deshmukh Government Medical College, Latur, Maharashtra, INDIA. 2Speciality Medical Officer, Vishnu Prasad Narayan Desai Hospital, Mumbai, INDIA. Email: babi.yadav8@gmail.com
Abstract Background: anaemia is known to cause CNS dysfunction and peripheral nervous system dysfunction. Aims and objectives: purpose of the study was to investigate the effects of anaemia on peripheral motor nerve function. Materials and Methods: A total of 100 patients with anaemia with age more than 12 years from department of medicine were taken as the study group. Patients with history of diabetes mellitus, peripheral nerve disease, pregnant females, and age less than 12 years were excluded from study. The motor nerve conduction parameters i.e. distal latency (DL), amplitude of compound muscle action potential (CMAP) and motor nerve conduction velocity (MNCV) were recorded bilaterally in median, ulnar, post. Tibial and common peroneal nerve using standard protocols. Values from patients were compared before and after treatment. Results: The motor nerve conduction velocities for both the Median and Ulnar nerves were significantly reduced in cases diagnosed as Megaloblastic anaemia. The distal latency for right Median nerve was found to be increased in cases with Megaloblastic anaemia. The nerve conduction parameters i.e. Motor Nerve Conduction Velocity (MNCV) improved significantly for the Median and Common Peroneal nerve after 6 months of treatment. Conclusion: Alteration in nerve conduction parameters in patients of anaemia and improvement in nerve conduction parameters at the end of treatment was reported in the present study. Key Words: motor nerve conduction velocity (MNCV), compound muscle action potential (CMAP)
INTRODUCTION Anaemia is reduction in oxygen carrying capacity of blood due to reduction in haemoglobin concentration. Anaemia is a global public health problem affecting both developing and developed countries with major consequences for human health as well as social and economic development. Anaemia is known to cause dysfunction of the central nervous system such as decline and slowing of cognitive functions, delayed growth and motor development and neurological symptoms such as paresthesia, weakness, clumsiness, and an unsteady gait. These are mostly due to loss of proprioception that may be attributed to reduced oxygen carrying capacity of the blood due to reduced levels of haemoglobin concentration in blood causing tissue hypoxia. Aims and Objectives: To study 100 patients of anaemia clinically and to find out any neurological involvement and to perform nerve conduction study in all the patients. To treat and follow all the patients for 6 months. To repeat nerve conduction study after 6 months.
MATERIALS AND METHODS Inclusion Criteria: All patients with age more than 12 years visiting the tertiary health center with haemoglobin less than 10 gm% in females and less than 11 gm% in males. Exclusion Criteria: pregnant females. Age less than 12 years. Anaemia with diabetes mellitus. All diseases known to give rise to neurological changes. History of peripheral nerve disease. Drug or alcohol addiction. Patient already on treatment. Sample Size: By using Convenience sampling the minimum sample size of 100 was utilized. Methodology: After approval from the Ethics Committee and with written informed consent, the eligible cases were enrolled in the study. Nerve is stimulated over 2 points and minimum distance between 2 points stimulation is 10 cm. Amplitude of CMAP is calculated as a point commencing at baseline to peak of negative deflection. Amplitude is recorded in millivolts (mv). Latency in milliseconds (ms) is measured from point of stimulus artifact to first negative deflection. Conduction velocity in meter per second is calculated by dividing the distance between two points with the difference between the two latencies.
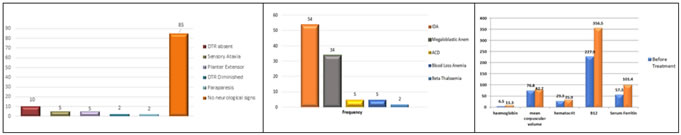
RESULTS Figure 1 Figure 2 Figure 3 Figure 4 Figure 1: Distribution of cases according to Severity of anaemia; Figure 2: Distribution of cases according to General symptoms; Figure 3: Distribution of cases according to general signs of anemia; Figure 4: Distribution of cases according to neurological symptoms of anemia In figure 3, It was observed that 9 (14.3%) cases with severe anaemia presented with absent Deep tendon reflex, followed by sensory ataxia in 5 (7.9%), Planter extensor in 4 (6.3%) and diminished DTR and paraparesis in 2 (3.2%) each respectively. Among those with moderate anaemia only 1 (2.7%) patient showed absent deep tendon reflex (DTR) and planter extensor respectively. Figure 5 Figure 6 Figure 7 Figure 5: Distribution showing neurological signs in cases of anemia; Figure 6: Distribution of cases according to Diagnosis; Figure 7: Distribution of hematological parameters before and after 6 months of treatment.
In figure 5, Most of the cases 2 (100.0%) with limb weakness, loss of balance 12 (92.3%), numbness 12 (60.0%) and paraesthesia 7 (50.0%) were diagnosed with Megaloblastic anaemia. Loss of balance was significantly associated with Megaloblastic Anaemia (p<0.001). In figure 6, Most of the cases 5 (100.0%) each with sensory ataxia and Planter extensors, Whereas 2 (100.0%) each with Diminished deep tendon reflexes (DTRs) and paraparesis were diagnosed with Megaloblastic anaemia. Absent deep tendon reflexes (DTRs) were present among 7 (70.0%) of the cases of Megaloblastic anaemia. Sensory ataxia (p=0.043) and planter extensor (p=0.043) were significantly associated with Megaloblastic Anaemia.
Table 1: Distribution of nerve conduction parameters of upper limbs before and after treatment
* p<0.05 is statistically significant
Table 2: Distribution of nerve conduction parameters of lower limbs before and after treatment
* p<0.05 is statistically significant
The motor nerve conduction velocities for both the Median and Ulnar nerves were significantly reduced in cases diagnosed as Megaloblastic anaemia (p<0.001). The distal latency for right Median nerve was found to be increased in cases with Megaloblastic anaemia (p=0.0001). There was a significant improvement in the hematological parameters of haemoglobin (HB), mean corpuscular volume (MCV), hematocrit (HCT), serum B12 levels and serum Ferritin after 6 months of treatment. The nerve conduction parameters i.e. Motor Nerve Conduction Velocity (MNCV) improved significantly for the Median and Common Peroneal nerves after 6 months of treatment.
DISCUSSION The present study was conducted among 100 cases of anaemia (Haemoglobin < 10 gm%) to assess the neurologic symptoms signs and the electrophysiological interaction of anaemia on peripheral nervous system and to investigate whether it is possible to reverse electrophysiological abnormality with appropriate treatment. The commonly reported neurological findings in the study by Divate et al. (2012) included numbness (13.9%), loss of balance (15.3%), absent Deep tendon reflexes (7.1%), and sensory ataxia (12%). It was observed that the commonest neurological manifestations included in present study is numbness in (20.0%), paraesthesia in (14.0%), loss of balance in (13.0%) and limb weakness in (2.0%) of them. Among the neurological signs, commonest was absent DTRs in (10.0%), sensory ataxia and planter extensors in (5.0%) each respectively. Loss of balance was significantly present among (19.0%) of the cases with severe anaemia (p = 0.03). In present study majority of the cases (54.0%) were diagnosed as Iron Deficiency Anaemia and 34.0% had Megaloblastic anaemia. In the present study, we conducted nerve conduction studies on both extremities. The median, ulnar, posterior tibial and common peroneal nerve, conduction parameters such as motor nerve conduction velocity (MNCV), compound muscle action potential (cMAP) and distal latency (DL) were measured. It was observed that the patients with Megaloblastic anaemia showed significantly reduced motor nerve conduction velocities for both the Median and Ulnar nerves (p <0.0001) along with prolonged distal motor latency, for right median nerve (p=0.0001). Similar results were reported by Kabakus et al.116 with regards to nerve conduction in the Median and Posterior Tibial nerves. The nerve conduction velocity and distal amplitude values in cases with anaemia were lower as compared with controls (those without anaemia). In another study by Swaminathan et al.120 the Ulnar, Median, and posterior Tibial nerves showed significant decline in the motor nerve conduction velocity (MNCV) and significant prolongation of distal latency (DL). When the nerve conduction parameters at baseline and after 6 months of treatment were studied, it was observed that the Motor Nerve Conduction Velocity (MNCV) improved significantly for the Median and Common Peroneal nerves (p<0.001) after 6 months of treatment. The change in the nerve conduction parameters from the current study is comparable to previous studies by kabakus et al. (2002) and Degirmenci et al. (2011). Nerve conduction velocities of both the median and common peroneal nerves in patients with anaemia improved significantly in the present study after 6 months of treatment. Axonal degeneration and demyelination are the major pathological changes that can affect the impulse conduction in a nerve. The iron deficiency anaemia involves central and peripheral nervous system enzymes like Mono-Amine Oxidase (MAO), catalase and cytochromes. The neurological dysfunction in iron deficiency is found to be linked with the deficiency of Mono-Amine Oxidase (MAO). Anemia induced peripheral neuropathy is a complex disorder in which the disease process may affect different type of nerve fibers to different degrees in every individual. Neuropathies are characterized by a progressive loss of nerve fibers, which may affect both principle divisions of the peripheral nervous system117. Anemia leads to decreased myelination, decreased rate and amount of neurotransmitter synthesis, thereby affecting the Nerve conduction Velocity (NCV) of peripheral nerves and increasing their latencies in anaemic individuals as compared to Non-Anaemic individuals118. There may be variability in the extent of dysfunction sensory nerve fibers. Some may show affliction of large sensory nerve fibers whereas, others may have a predominantly small-fiber neuropathy.
CONCLUSION Our study confirms the involvement of peripheral nerves in anaemia. Nerve conduction study showed impairment in conduction velocity even without neurological symptoms as well as neurological manifestations. Thereby emphasizing that early nerve conduction study can be advised as neurological symptoms and signs appear late in course of anaemia or with severe anemia. There was improvement in hemoglobin and nerve conduction velocity at the end of 6months treatment. Thus early identification of neurological changes with the help of Nerve conduction study (NCS) and prompt treatment of anaemia is mainstay for managing neurological manifestations in anemia.
REFERENCES
Policy for Articles with Open Access
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
 Home
Home